Background
Depression is the largest contributor to disability among all mental and substance abuse disorders, not only amounting to serious personal difficulties, but also social, economic and societal costs. Digital interventions for depression, such as, internet-delivered Cognitive Behavioral Therapy (iCBT) are a well-established and evidence-based option for the treatment of depression. Monitoring of daily activities and experiences, involved in behavioural activation, is a core tenet of CBT for depression. Insights from monitoring help both patients and therapists identify the patterns between a patient’s behaviour and their mood in order to improve outcomes. For example, sleep problems can often co-occur with depression while moderate levels of physical exercise can improve depression symptoms.
Wearable technologies, such as smartwatches, are increasingly popular and used by many in the general population to monitor their own behaviours during activities such as sleep or exercise. These wrist-worn smartwatches facilitate the immediate and automatic collection of health data through sensors and lead to questions about their potential to provide more accurate and complete monitoring in therapeutic settings. However, as with any technology-delivered treatment, success and compliance is based on how acceptable the patients view the technology.
Objective
The aim of this study is to explore how acceptable is the use of a smartwatch app, for self-monitoring of mood, sleep and activity level, when integrated as part of an established iCBT programme for depression. A secondary aim will be to explore if the integration of the smartwatch leads to differences in terms of engagement with the programme or clinical outcomes.
Method
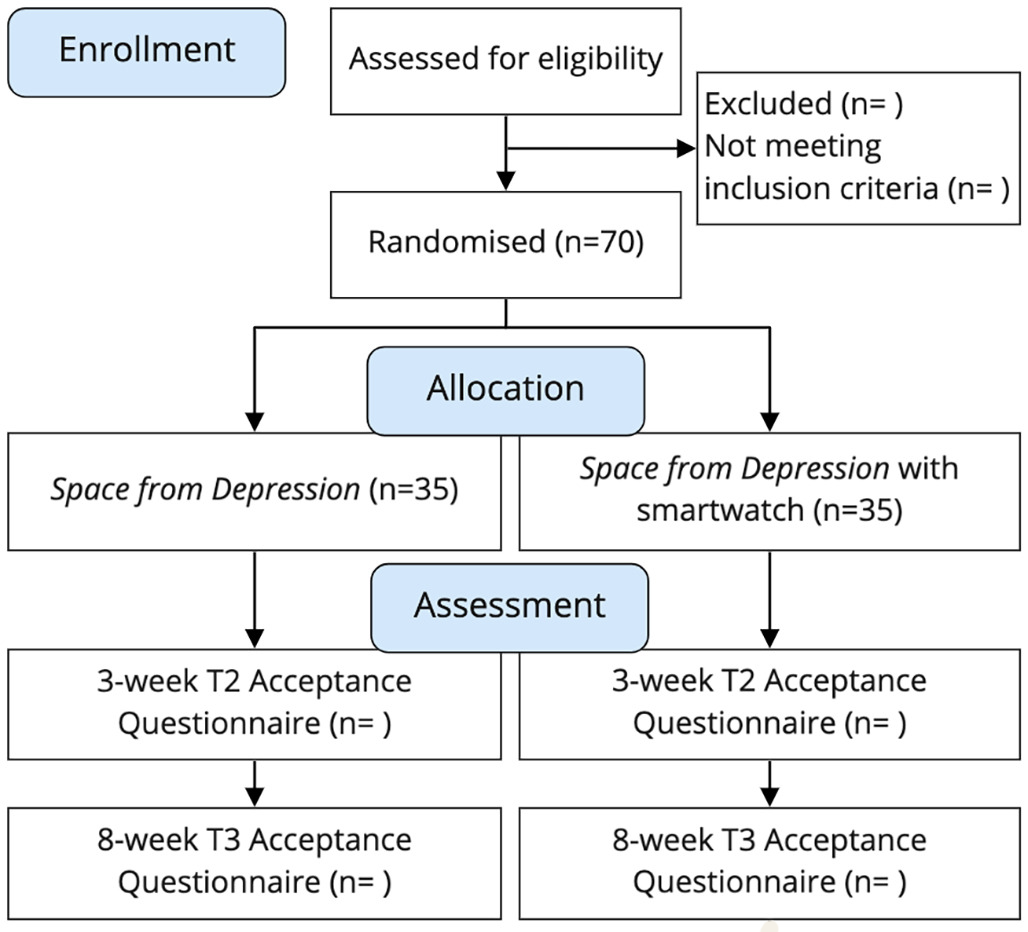
The study will be conducted within the Improving Access to Psychological Therapies (IAPT) in the UK, which is a stepped care model for the treatment of common mental health disorders, such as depression and anxiety. Specifically, service patients with mild to moderate levels of depression and anxiety who are referred to step 2 and are assigned to the ‘Space from Depression’ programme will be invited to participate. Within this context, the programme is offered with support from a trained clinician.
Individuals will be randomized to one of two groups: a) standard ‘Space from Depression’ b) ‘Space from Depression’ plus smartwatch app. Participants will be evaluated in terms of how they perceive the smartwatch app’s usefulness, ease of use, their attitude towards it, intention to use, and actual usage over time.
The smartwatch app
The smartwatch app contains the mood monitor tool that is part of the ‘Space from depression’ programme which records patients’ mood, sleep, and physical activity. The smartwatch app integration is composed of a Mood Monitor and Lifestyle Choices chart. There are daily and weekly visualisations of the user’s mood, bedtime, number of hours slept, and step count. Other supportive features include colourful changing icons, directional arrows highlighting changes in behaviour from the previous day, positive reinforcement through encouraging prompts for positive engagement, and educational information regarding lifestyle choices drawn from the iCBT programme. Examples of a variety of smartwatch screens can be seen in Figures 1 and 2. Mood, sleep, and physical activity logged will be integrated into the patient’s SilverCloud account and shared with their supporter.
Conclusions
Patient acceptance is crucial for successful digital mental health interventions to avoid their rejection or discontinuation. The increased ease of access in recording behaviours, greater specificity of reminder-setting, and improved feedback and visualisation of behaviours over time may facilitate usage and engagement with the iCBT treatment for depression. In-the-moment assessments facilitated by wearable technologies increase accuracy and completeness of data collection which can help inform our understanding of the relationship between mood, behaviours, and clinical outcomes. In addition, automatic monitoring of sleep or activity levels can lessen the patient’s burden of remembering to report. Ultimately, the findings of this trial will contribute to assessing the utility of a smartwatch in self-monitoring within a clinical setting as well as factors that impact patient engagement.
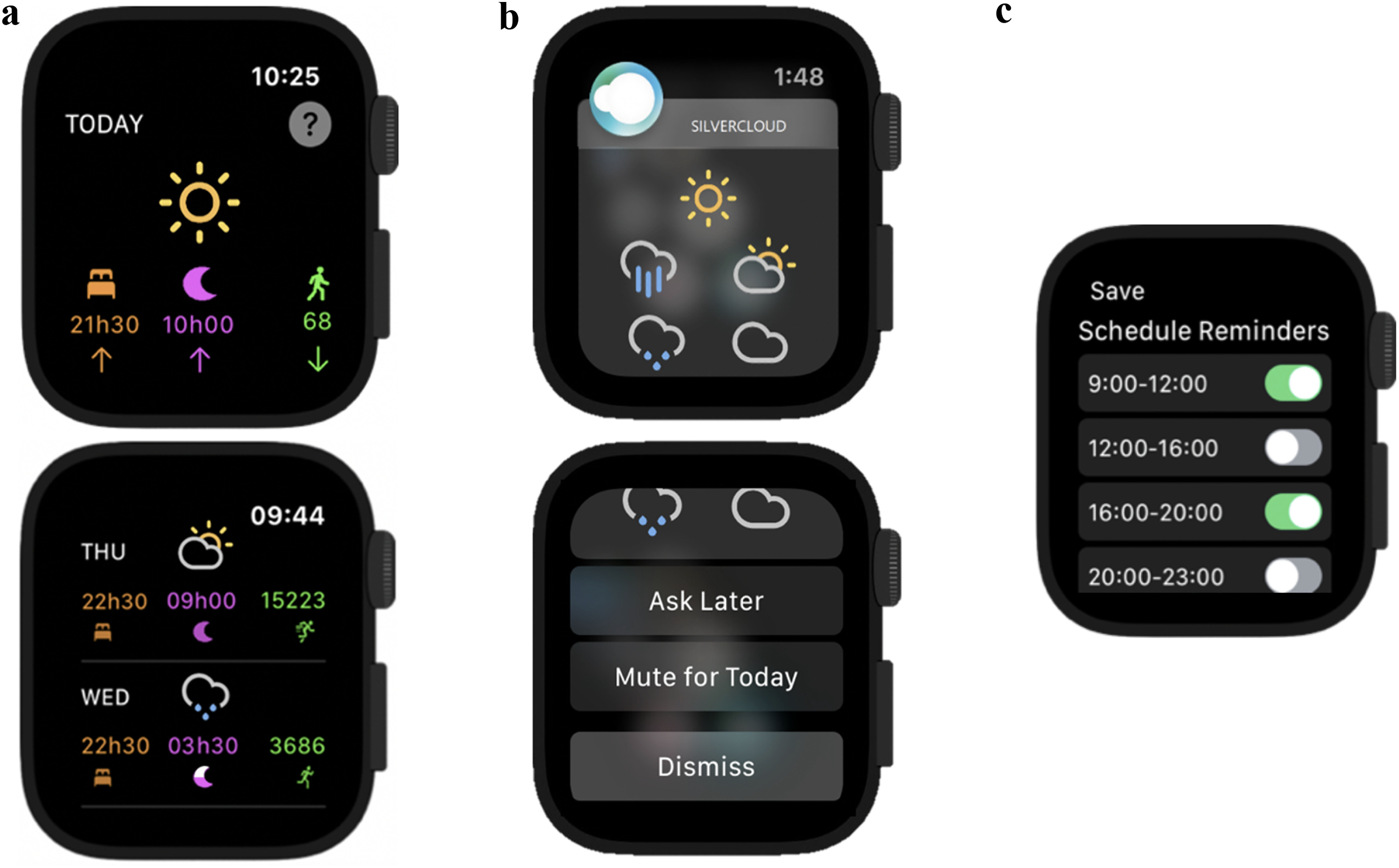
Figure 1. a) Home screen. b) Mood reminder. c) Reminder scheduling.

Figure 2. a) Encouraging prompts. b) Tips to stay well.
Acknowledgements
We would like to thank Berkshire Healthcare NHS Foundation Trust for their collaboration in this study, particularly the Principal Investigator Sarah Sollesse and her team of psychological wellbeing practitioners.
This work was jointly supported by AffecTech: Personal Technologies for Affective Health, Innovative Training Network funded by the H2020 People Programme under Marie Skłodowska-Curie grant agreement number 722022, and SilverCloud Health. This research was supported, in part, by Science Foundation Ireland grants 13/RC/2106 (Adapt) and 13/RC/2094 (Lero).









